AnswersPublished8 sources
你是一個ivf expert , 這個女人今天要移植,子宮內膜上超聲波獻示疑似有液體, 還能移植嗎
不建議今天進行胚胎移植。 如果超音波確認子宮內膜腔有液體(endometrial cavity fluid, ECF),尤其是移植當天仍持續存在,多數文獻與常見臨床做法都傾向取消本次移植、密切追蹤或改採後續冷凍胚胎移植(FET)策略。[2][4][5] 這樣做的目的,是先評估可能原因(如輸卵管積水、PCOS、亞臨床子宮感染等)並處理,等下次週期子宮腔乾淨後再移植。[2][3] 若液體在移植前自行消失,後續FET的活產率可與從未出現ECF者相近。[3][4] 最終決定必須由您的
824K0
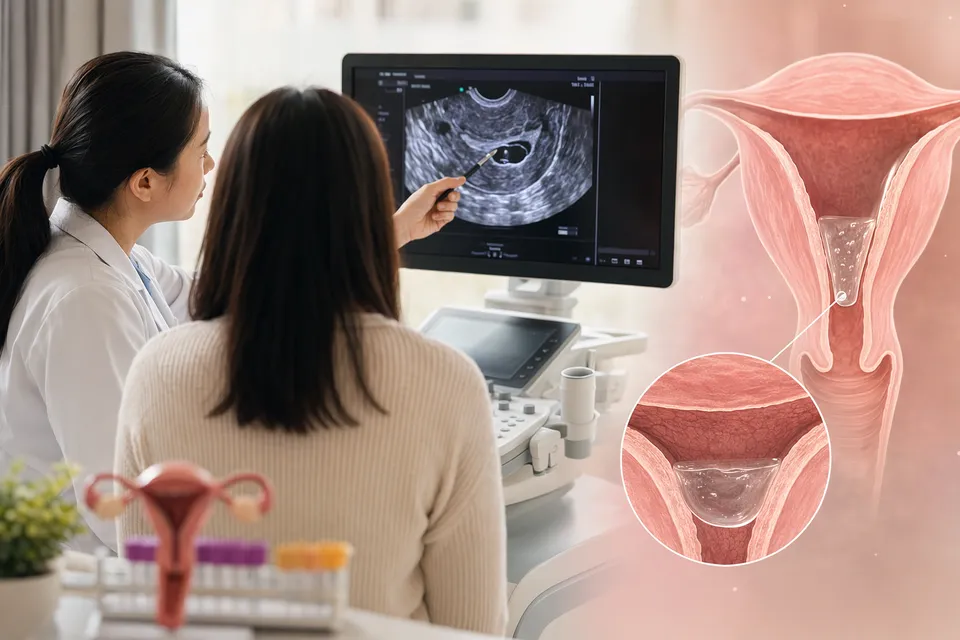
AI Prompt
openai.comCreate a landscape editorial hero image for this Studio Global article: 你是一個ivf expert , 這個女人今天要移植,子宮內膜上超聲波獻示疑似有液體, 還能移植嗎. Article summary: 不建議今天進行胚胎移植。 如果超音波確認子宮內膜腔有液體(endometrial cavity fluid, ECF),尤其是移植當天仍持續存在,多數文獻與常見臨床做法都傾向取消本次移植、密切追蹤或改採後續冷凍胚胎移植(FET)策略。[2][4][5] 這樣做的目的,是先評估可能原因(如輸卵管積水、PCOS、亞臨床子宮感染等)並處理,等下次週期子宮腔乾淨後再移植。[2][3] 若液體在移植前自行消失,後續FET的活產率可與從未出現ECF. Topic tags: deepresearch, general web, workflow, security, privacy. Reference image context from search candidates: Reference image 1: visual subject "cycle is endometrial fluid. This is fluid seen inside the uterine cavity and might come from mucus, blood, inflammatory secretions, or fluid from the fallopian tubes. Doctors usual" source context "Researchers examine how endometrial fluid before transfer affects live birth rates" Reference image 2: visual subject "However, Strandell _et al._ ([20](https://pmc.ncbi.nlm.nih.gov/article
不建議今天進行胚胎移植。 如果超音波確認子宮內膜腔有液體(endometrial cavity fluid, ECF),尤其是移植當天仍持續存在,多數文獻與常見臨床做法都傾向取消本次移植、密切追蹤或改採後續冷凍胚胎移植(FET)策略。[2][
4][
5] 這樣做的目的,是先評估可能原因(如輸卵管積水、PCOS、亞臨床子宮感染等)並處理,等下次週期子宮腔乾淨後再移植。[
2][
3] 若液體在移植前自行消失,後續FET的活產率可與從未出現ECF者相近。[
3][
4] 最終決定必須由您的主治醫師依據即時影像、液體量、內膜厚度、週期類型(新鮮或解凍)與完整病史判斷;這不是個人化醫療建議,請立即與您的醫生討論。
Studio Global AI
Search, cite, and publish your own answer
Use this topic as a starting point for a fresh source-backed answer, then compare citations before you share it.
Key takeaways
- 不建議今天進行胚胎移植。 如果超音波確認子宮內膜腔有液體(endometrial cavity fluid, ECF),尤其是移植當天仍持續存在,多數文獻與常見臨床做法都傾向取消本次移植、密切追蹤或改採後續冷凍胚胎移植(FET)策略。[2][4][5] 這樣做的目的,是先評估可能原因(如輸卵管積水、PCOS、亞臨床子宮感染等)並處理,等下次週期子宮腔乾淨後再移植。[2][3] 若液體在移植前自行消失,後續FET的活產率可與從未出現ECF者相近。[3][4] 最終決定必須由您的
People also ask
「你是一個ivf expert , 這個女人今天要移植,子宮內膜上超聲波獻示疑似有液體, 還能移植嗎」的簡短答案是什麼?
不建議今天進行胚胎移植。 如果超音波確認子宮內膜腔有液體(endometrial cavity fluid, ECF),尤其是移植當天仍持續存在,多數文獻與常見臨床做法都傾向取消本次移植、密切追蹤或改採後續冷凍胚胎移植(FET)策略。[2][4][5] 這樣做的目的,是先評估可能原因(如輸卵管積水、PCOS、亞臨床子宮感染等)並處理,等下次週期子宮腔乾淨後再移植。[2][3] 若液體在移植前自行消失,後續FET的活產率可與從未出現ECF者相近。[3][4] 最終決定必須由您的
下一步適合探索哪個相關主題?
繼續閱讀「螞蟻集團獲利暴跌79%的真正原因:AI豪賭與全球擴張正在重塑公司」,從另一個角度查看更多引用來源。
Open related page我應該拿這個和什麼比較?
將這個答案與「SpaceX 星艦第12次飛行測試:Starship V3 首次發射與關鍵看點」交叉比對。
Open related pageContinue your research
Sources
- [1] Effect of Endometrial Cavity Fluid On Pregnancy Rate of Fresh ... - NIHpmc.ncbi.nlm.nih.gov › articles › PMC5799933pmc.ncbi.nlm.nih.gov
All patients selected in the study had grade-A embryo transfer of day 3–4 with maximum three embryo transferred. Pregnancy was defined by rising serum beta-human chorionic gonadotrophin levels performed after 14 days of embryo transfer and further confirmed...
- [2] Fluid Within the Endometrial Cavity in an IVF Cycle—A ...pmc.ncbi.nlm.nih.gov
Fluid within the endometrial cavity before embryo transfer in IVF cycles is associated with failure of implantation. The etiology of endometrial fluid is surrounded in controversy but it is associated with hydrosalpinges, polycystic ovarian disease, and sub...
- [3] Live birth rates after resolution of endometrial cavity fluid in ...pmc.ncbi.nlm.nih.gov
Live birth rates in frozen embryo transfer cycles are equivalent between patients with resolved endometrial cavity fluid compared to those who never had endometrial cavity fluid. Our findings suggest that the presence of endometrial cavity fluid is likely n...
- [4] Live birth rates after resolution of endometrial cavity fluid in frozen embryo transfer cyclesncbi.nlm.nih.gov
Perhaps the most common approach, adopted by our centre, includes expectant management with close ultrasound surveillance to determine if ECF remains present on day of transfer. If persistent the embryo transfer would be cancelled, but if resolved then tran...



